Sex. The primal human need we are all trying to satiate but, in hyper-religious societies like Nigeria, will rather have remain cloaked in secrecy.
At over 200 million, the country’s youth bulge stays growing. According to 2019 data from the United Nations Population Fund (UNFPA), Nigerians aged 15 to 64 now make up the majority of the population at 54% and within this age bracket lies a human’s best reproductive years.
How did your first sex education go? It may have been your parents trying to summarise the entirety of reproductive health and sexual intimacy in a 30 minute cryptic talk that left you feeling confused or threatened.
It may have been at school with teachers dancing between trying to pass on just enough information and not going into much useful detail to kickstart your imagination. Or, the Internet, the seeming know-it-all of everything under the sun.
What these measured dishing out of information has done is deepen the culture of secrecy around sexual and reproductive health so that they are still approached as taboo topics and often elicit judgemental looks and speeches when not aligned with what prevalent culture and religious leanings accept as normal, even from healthcare workers.
Take contraceptive use in Nigeria. As it stands, the variety available for men remain limited to male condoms and vasectomy. Women tend to be the ones with a gamut of options to choose from but with little access or information to these options.
The UNFPA says only 15% of women in Nigeria use modern contraceptive methods (19% used any at all). But between 2006-2017, adolescent birth rates in the country among girls aged 15-19 stood at 145 per 1,000 girls, one of the top ten countries surveyed.
When Morenike Fajemisin started toying with the idea to start WHISPA Health, these were the issues she wanted to tackle.
Not many young adults, male or female, can walk into a pharmacy to buy a pack of condoms or contraceptives of any kind because pharmacists or staff on the other side of the counter expect you to not be sexually active as an unmarried individual let alone to flaunt it boldly.
But the scales are even more tilted against young adult women.
Tola*, 29 and married, tells TechCabal a pharmacist once told her he would sell her emergency contraceptive pills the one time and “I should not come back.”
“It was a very busy pharmacy but time was ticking,” Miriam* another young woman in her late twenties says of her experience with buying an emergency contraceptive.
“I just walked to the counter and showed her [pharmacist] a picture from Google and said, do you have this? She said yes and packed it and gave me.”
“Young people will try to whisper and do their best to ensure that no one hears what they are trying to buy,” Fajemisin recalls from her days as a community pharmacist when she spoke with TechCabal.
“If they end up in a pharmacy where someone is shouting back their request at them, I have seen someone turn around and dash out of the pharmacy embarrassed.”
Alongside two co-founders, Fajemisin launched the WHISPA app in April to address two key areas; discrete access to quality sexual health information and access to quality sexual and reproductive health resources.
“I knew where all these services were by virtue of my career and I wanted to use technology to ensure that access is available to everyone and not just people in the know like myself,” she says.
Although serving both males and females, the user base on the WHISPA app is predominantly female (60-65%) and comprises really young individuals typically still in undergraduate study or just young school leavers yet to begin their first real out-of-school jobs. The app was supposed to address women’s issues the most, Fajemisin says, and that is what they have seen in practice.
WHISPA offers help to their users with two major features: a telemedicine platform which allows users discreetly chat with certified medical professionals about sexual and reproductive health related matters and secondly, a contraceptive feature that allows women take automated tests to determine what contraceptives suit them and have it delivered or picked up.
“We currently have four doctors on our platform to ensure fast response time,” Fajemisin says.
“Our doctors are youth-friendly and carefully selected to ensure they are health providers who align with our shame-free, stigma-free culture at WHISPA.”
To pay heed to strict regulatory requirements to offer the kinds of services it does, the company partners with licensed doctors, registered hospitals, pharmacies and pharmaceutical companies. Fajemisin says the goal is to review these partnerships on an annual basis “to weed out anyone who is no longer compliant”.
So far, the company has been self-funded. Some external funding have come by way of an “ingenuity fund” grant from John Hopkins University.
“At the moment, we are in our seed round of funding and are on the look-out for investors.”
Even with its lean purse, the company has allocated a substantial amount to data privacy and security, a very important aspect of the increasing tilt towards technology-powered healthcare solutions.
“We have invested in using Amazon’s AWS platform for our data security and storage. It might be expensive for a startup to use AWS, but we believe it is worth it as we do not take data security lightly,” Fajemisin explains.
Currently, all users on the platform are part of a basic plan where consultations are tiered at ₦250($0.5)/consultation (a consultation entails asking /chatting with a doctor about one question) or a bundle of five consultations at ₦1,000($2.12) and 10 at ₦1,800($3.83). The costs reflect the user base and how much they are able to afford to access the services.
Technology tools have become a beacon in Africa for what could possibly better a healthcare system greatly challenged by infrastructure and personnel deficits.
Tools like WHISPA proffer useful sexual health guidance to young adults in conservative countries like Nigeria where discreet access to sexual health tools and information can meet already innate behaviours around the use of these digital tools. Last year, NOIPolls found that 60% of young Nigerians spend 4-6 hours on social media platforms daily. A small percentage spent more, north of 10 hours daily on platforms like Twitter and WhastApp.
“When it comes to sexual health, technology [tools] such as WHISPA mobile app is even more of a game changer, [in that it is] providing young people (women in particular) with the kind of ease of access to sexual healthcare that addresses their needs for privacy or even anonymity without shortchanging them on quality of care,” Fajemisin says.
Honey&Banana Connect, another such tool, is a digital hub set up by family planning non-governmental organization, DKT International. Accessible through a toll-free call center (with the exception of GLO subscribers), SMS, web and mobile apps, and instant messages, the hub provides individuals with discreet and private access to sexual health information and advice as well as resources. Coupled with its offline product/ service delivery points like partner clinics, pharmacies and chemist shops, the hub provides physical appointments and pickup of products to customers at access points of their choosing.
Perhaps, because healthcare workers in these physical locations have been trained to shed their biases when interacting with young Honey&Banana Connect customers in person, younger callers prefer to visit pharmacies and clinics to get their contraceptives. On the flip side, taking delivery of contraceptives at home where they can be intercepted by parents or other adults can also be driving this pattern.
“The Honey&Banana website and brand was designed with youths in mind to avoid the stigma associated with searching for family planning or sex-related information,” Chidinma Onuoha, Program Director, Honey&Banana Connect, tells TechCabal.
Since its launch in 2016, the website has been visited over 172 million times (mostly by individuals between the ages of 15 and 29), and agents have responded to over 86,000 family planning-related questions across the web platform and its social media channels. Inbound calls into the contact center can range anywhere from 500 to 1,500 per day depending on whether there are active marketing campaigns ongoing or not.
As with WHISPA, Honey&Banana’s predominant visitors are female making up 70% of the audience. The age demographic is similar as well with the platform serving young Nigerians between 15 and 35 mostly.
But what is more enlightening about the numbers at Honey&Banana Connect is the quality of data the digital tools are able to shore up really quickly regarding the dynamics and use of contraceptives among younger Nigerians. As Onuoha says, increasingly, more and more young people are asking questions about family planning methods.
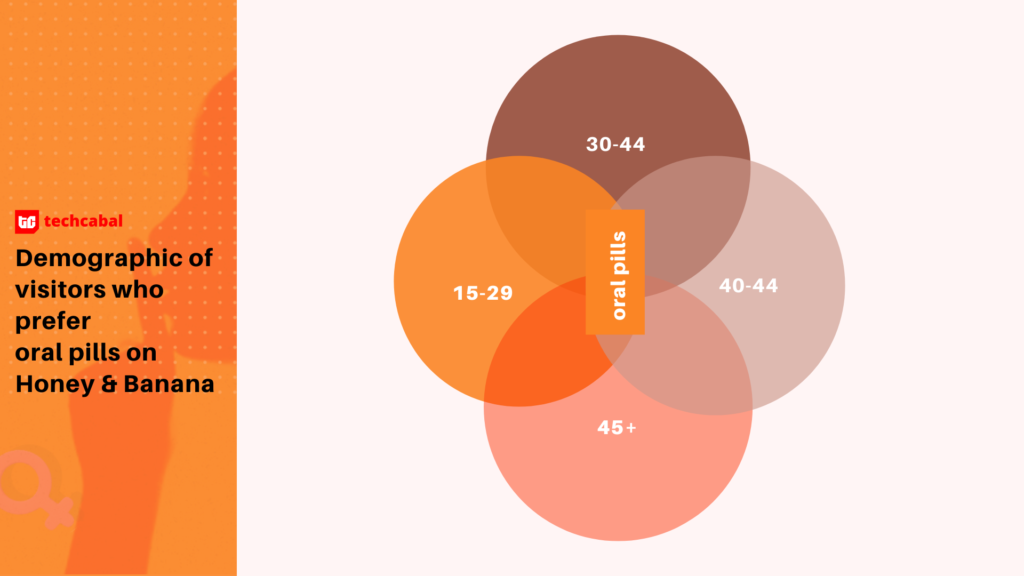
The challenges are similar: young people are often met with bias when they approach healthcare personnel or institutions for information around sex and contraceptive and are often left with their myths and misconceptions.
In addition to this, regulatory restrictions around what can be advertised during certain call times has proved to be challenging to the digital hub. But its impact is still incredibly powerful and indicative of what is possible with such tools.
“In October 2020, DKT distributed over 14 million condoms; 8,500 inter uterine devices (IUDs); 15,400 contraceptive injections; 289,000 oral contraceptive pills (OCPs); 198,000 emergency contraceptive pills, and 13,900 HIV self-test kits,” Onuoha told TechCabal.
The goal is not just to prevent the spate of unwanted pregnancies in a country where abortion remains illegal, but very importantly, reduce the risks of contracting and disseminating sexually transmitted diseases (STDs).
Adequate knowledge remains critical in the development of sexual behaviors and patterns that control the spread and risk of infections.
Update: The article has been updated with comments from Honey & Banana Connect.




















